Skin cancer
Skin cancer has become a very important topic in recent years. More and more people are suffering from one or the other form of skin cancer or a skin cancer precursor. In recent decades, there has been an exorbitant increase in skin cancer cases - a doubling of affected patients has been observed every 10 years.

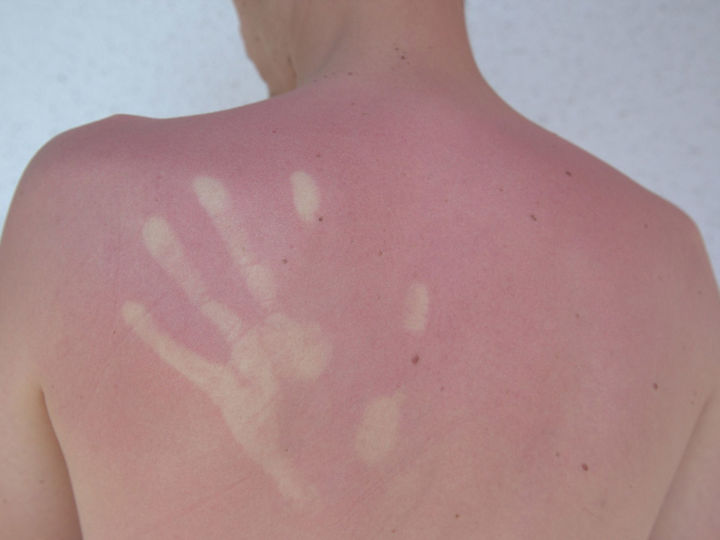
The sun is the main cause of skin cancer
The sun, which brings us so many beautiful hours around the world, is essentially responsible for the fact that skin cancer is one of the most common forms of cancer. However, under the general term skin cancer, very many very different diseases are subsumed; These diseases sometimes differ greatly in the type of therapy needed and their overall prognosis.
Skin cancer: easy to treat
Nearly all forms of skin cancer can be treated well by a consistent early detection. All modern diagnostic procedures and therapy options are available for this purpose. Depending on the type of tumor, there are a variety of different treatment options, from a local treatment with creams or a surgical removal up to modern systemic therapies like immune therapy or targeted chemotherapy.

Dermatologist Robert Loewe: Your specialist for skin cancer
Due to my many years of experience in the diagnosis and treatment of skin tumors I am familiar with all of these sometimes very peculiar and sometimes rare diseases and I am able to take care of you and support you in difficult situations.
Skin cancers
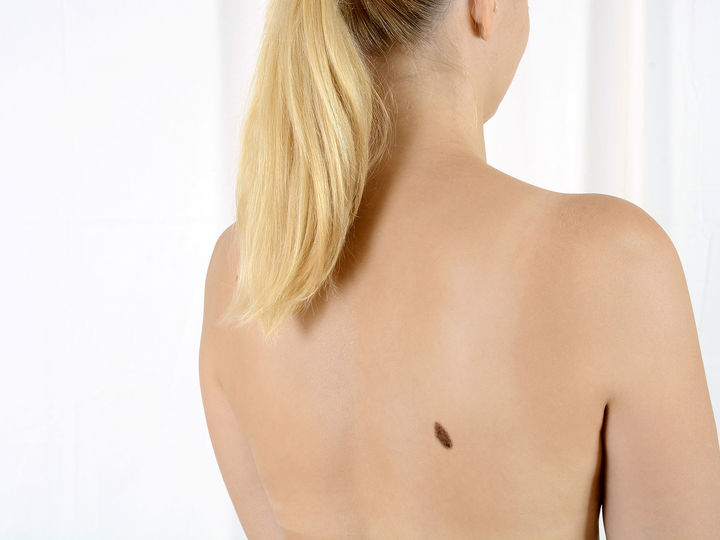
Black skin cancer (melanoma)
Melanoma is a highly malignant tumor derived from pigment cells (melanocytes). Damage to the skin due to UV radiation plays an important role in many cases of melanoma. The tumor tends to spread, early metastases may develop via lymph and blood vessels and is therefore considered extremely dangerous.
With an early diagnosis and treatment, the chances of a cure are good. Hesitating or waiting, whether due to negligence or anxiety, worsens the outlook significantly.
The most important form of therapy is the surgical removal of the primary tumor. Decisive for the further prognosis of the illness is the examination of the tumor material and the lymph nodes of the adjacent regions. Especially in recent years there has been dramatic progress in the treatment of advanced melanoma (metastasized melanoma). New forms of therapy, such as immunotherapy and targeted therapy, have significantly improved the prognosis of the affected patients. I am well acquainted with all of these therapies, and my work at the Department of Dermatology as Senior Consultant of the Consultation Center for Rare Skin Tumors and the Oncology Outpatient Clinic also provides access to the most recent clinical trials.
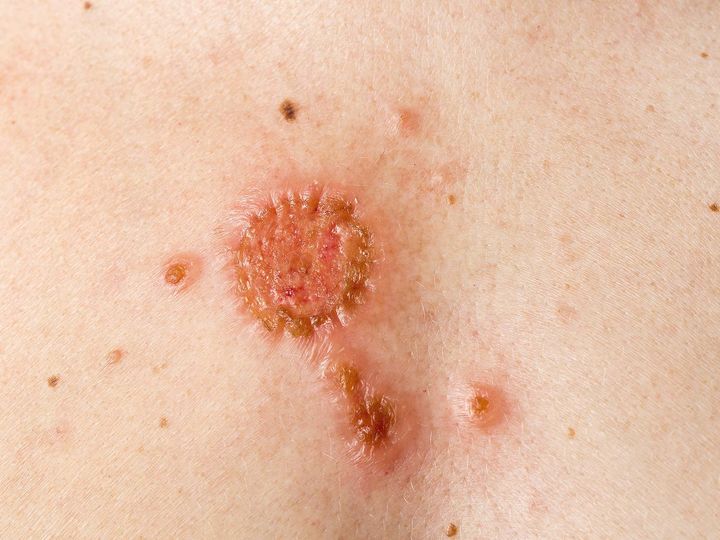
“White skin cancer” (basal cell carcinoma)
For a long time the surgical removal of the tumor was the gold standard of treatment. This is still the case today for deep penetrating tumors. However, for the treatment of superficial basal cell carcinomas, especially in the facial area, the most modern forms of therapy without surgery are available. Local therapy using an immunomodulating preparation or photodynamic therapy (PDT). Using PDT, several sessions are usually necessary for complete removal of the tumor. These local therapies often save surgical treatments, especially in the facial area, where we must not lose sight of the aesthetics. When the first step of therapy, the removal of the tumor, is completed, we conduct regular follow-up visits to detect and treat any emerging malignant lesions early on. Of course, we recommend the application of special sunscreens, adjusted to the individual skin type, for further prevention. In the rare event that a basal cell carcinoma is already significantly advanced locally and is therefore no longer available for surgical or local therapy, there is a drug therapy, which leads in most cases to a significant reduction in tumor area. Our ordination has many years of experience with this systemic "hedgehog inhibitor" therapy.
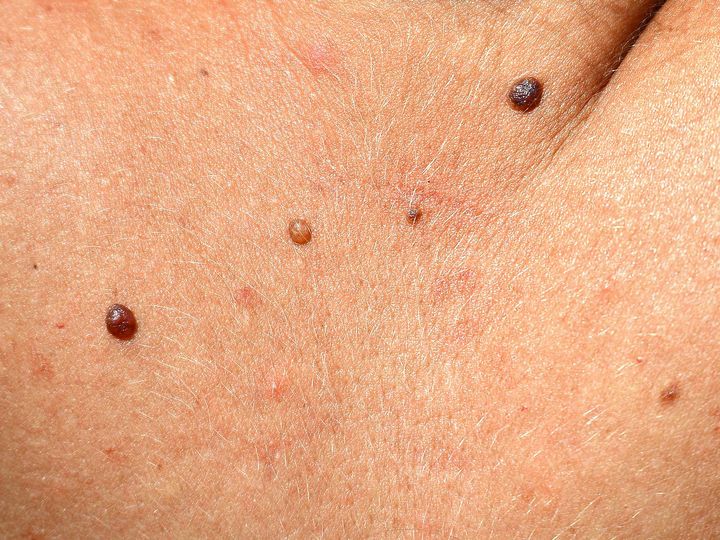
Actinic keratoses
In heavily photodamaged skin (face, bald, forearms and hands) and with certain predisposition, so-called "actinic keratoses" often develop in older people. These are sharply defined, reddened areas of the skin, which usually carry a firmly adhering dandruff. They are often considered to be "dry skin". Squamous cell carcinoma can evolve on the basis of these changes - but this does not have to be the case with every patient. Actinic keratoses can be removed very easily by local measures such as cold, ablation, various local therapies or photodynamic therapy or the use of lasers. However, the damage always affects a larger area (“field damage”), this is the reason why affected people need to be monitored regularly and treatments have sometimes to be repeated.
cutaneous squamous cell carcinoma
Squamous cell carcinoma is the second most common skin cancer. The highest risk of developing squamous cell carcinoma possess fair-skinned people. It mainly affects older people who have been exposed to the sun for many years (decades). Unfortunately, squamous cell carcinomas are also increasingly affecting younger patients due to the changed leisure habits. In addition to permanent exposure to natural light, radioactive radiation, radiation treatments (light and X-ray radiation), chronic inflammation and particularly pronounced scars can be causally involved in the development. Organ transplants or immunosuppression (illness or medication-related inhibition of the immune system) additionally increase the risk for the development of squamous cell carcinoma of the skin manyfold.
Squamous cell carcinomas are malignant skin tumors, which through local unrestrained growth destroy adjacent structures and thus cause great damage. By early, complete removal, squamous cell carcinomas of the skin can usually be finally and completely cured. Dislocation into distant organs (metastasis) is relatively rare in squamous cell carcinoma of the skin, but more common in thicker primary tumors or at specific anatomical sites like earlobes, lips, genital area. The highest risk for metastasis exists in the immunosuppressed patient, e.g. after organ transplants. Therefore, it is extremely important to contact us even with the smallest unclear change of the skin. Thus, in most cases, by early detection and treatment, we can avoid dire consequences.